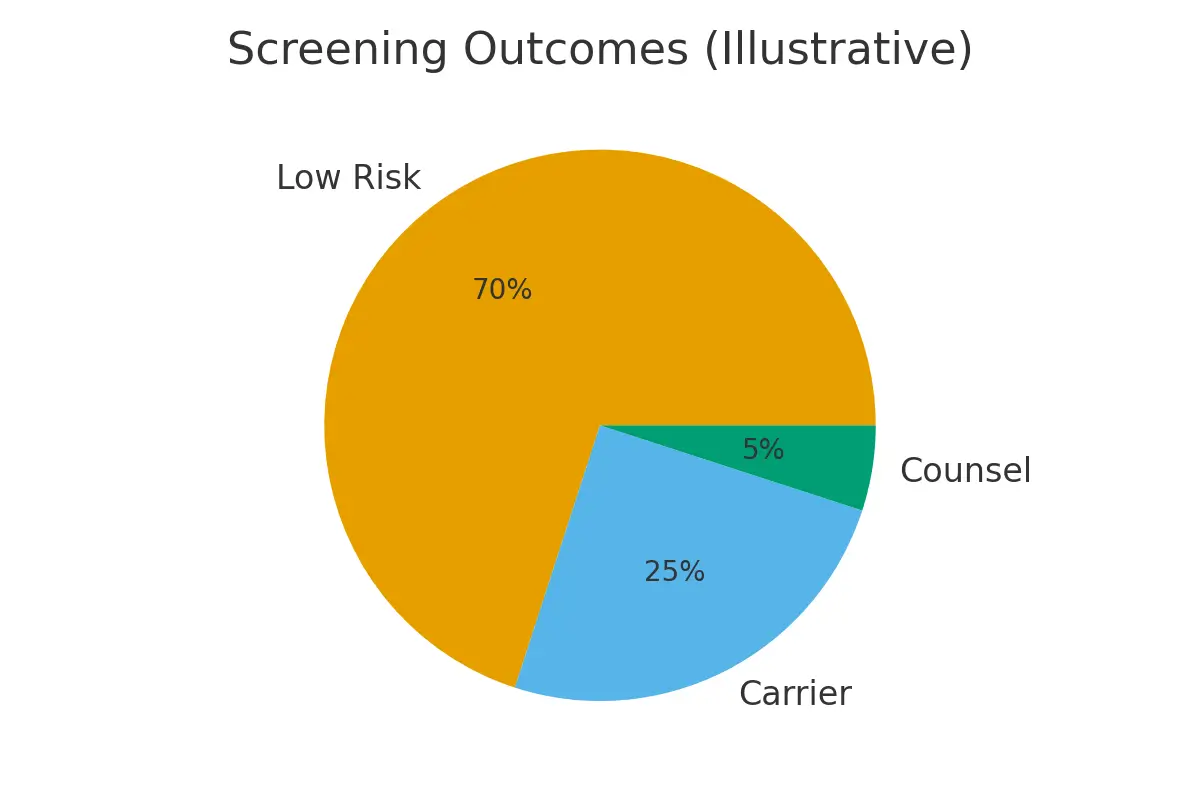
HLA (Human Leukocyte Antigen) matching refers to testing embryos for compatibility with an existing child who needs a stem-cell or bone-marrow donor. It’s typically paired with PGT-M or PGT-A and used to ensure that a future baby can safely donate cord blood or bone marrow to a sibling with a life-threatening condition.
This section explains:
- Where HLA matching fits in the IVF + genetic testing process
- What it changes (embryo selection strategy, lab timelines, success expectations)
- How upstream choices—like panel selection and cycle timing—shape downstream results such as embryo availability and transplant planning
- The ethical framework clinics use when balancing the needs of the current child with the welfare of the future child
Who It Helps
Signals this pathway is a good fit
- You have a child with a genetic or hematologic condition requiring stem-cell transplantation (e.g., thalassemia, sickle cell disease, immunodeficiencies).
- You’re planning IVF for medical reasons and want to combine PGT-M with HLA matching.
- Your care team indicates that an HLA-matched sibling donor would significantly improve treatment outcomes.
- You need a predictable, stepwise path to coordinate fertility care with hematology/transplant teams.
When to consider a different path
- The existing child does not require stem-cell or cord-blood transplant.
- You prefer to avoid embryo testing due to ethical, cultural, or religious considerations.
- IVF is not medically or financially feasible at this time.
- There is an available matched unrelated donor or haplo-donor, making sibling matching unnecessary.
Step-by-Step: A Simple, Clear Process
-
Consult hematology + genetics together
Align on diagnosis, transplant urgency, and whether HLA matching will materially improve outcomes. -
Complete both partners’ genetic panels
If a single-gene condition is involved, confirm which mutations must be excluded during PGT-M. -
Develop a combined PGT-M + HLA testing assay
This step takes 4–8+ weeks and must be completed before starting an IVF cycle. -
IVF cycle + embryo biopsy
Embryos are tested for:-
HLA match
-
Presence/absence of the relevant disease mutation
-
(Optional) chromosomal status (PGT-A)
-
-
Review results in a coordinated meeting
Decision tree:-
Embryo is mutation-free + HLA-matched → eligible for transfer.
-
Mutation-free but not HLA-matched → may be kept or discarded depending on family goals.
-
Affected embryos → excluded.
-
-
Plan transfer timing
Align with hematology on transplant timeline and cord-blood collection logistics. -
Document thresholds
Decide:-
How many attempts you’re willing to pursue
-
Acceptable alternative donor strategies
-
Budget and time limits
-
This structure reduces stress and avoids rushed, emotion-driven decisions.
Pros & Cons
Pros
- Gives the best chance of finding a compatible donor for a child in need.
- Allows simultaneous screening for single-gene disorders.
- Enables coordinated planning with transplant teams.
- Cord-blood collection is noninvasive and high-yield.
Cons
- Lower probability of obtaining an HLA-matched, disease-free embryo (match rate ~1 in 4 even before PGT filtering).
- IVF + testing timelines may delay treatment if urgency is high.
- Emotional pressure on the family regarding the future child’s role.
- Cost and complexity of combined PGT-M + HLA assays.
Costs & Logistics
Typical line items
- PGT-M + HLA assay development: $4,000–$8,000
- PGT testing per embryo: $300–$600
- IVF cycle costs: varies by clinic
- Genetic counseling: $0–$250
- Cord blood banking/processing: $1,500–$3,500
Insurance considerations
- Medical necessity may apply depending on the existing child’s diagnosis.
- Prior authorizations are essential and may take 2–4 weeks.
- Keep all documentation from hematology to support insurance appeals.
Cash-flow management
- Track three parallel bills:
IVF clinic / Embryology lab / Genetic testing company - Ask for written cost caps before assay development begins.
What Improves Outcomes
High-impact actions
- Early joint consult with hematology + IVF genetics team.
- Starting assay development before ovarian stimulation.
- Planning for multiple cycles if needed (low match probability).
- Managing expectations about timelines and probabilities.
Low-impact or unnecessary actions
- Repeating carrier screening panels.
- Running HLA matching without confirming the diagnosis driving the need.
- Prioritizing PGT-A alone (it does not influence HLA match success).
Case Study
A family’s daughter had beta-thalassemia major requiring regular transfusions. A matched unrelated donor search failed. Their hematologist recommended IVF with PGT-M + HLA matching.
Process:
- Assay development: 7 weeks
- IVF cycle: 12 eggs → 7 blastocysts
- Combined testing:
- 3 embryos were disease-free
- 1 of those 3 was also an HLA match
The matched embryo was transferred in a frozen cycle.
Cord blood collected at birth was used for transplant at 7 months of age.
The child engrafted successfully, and the older sibling is now transfusion-independent.
This case illustrates how clear thresholds, good communication, and early planning turn a complex scenario into a predictable, coordinated pathway.
Mistakes to Avoid
- Starting an IVF cycle before the HLA/PGT-M assay is complete.
- Assuming every embryo has a high chance of being a match—probability is low.
- Not involving the hematology team early.
- Overlooking emotional and ethical considerations in counseling discussions.
- Ignoring backup donor options in case no HLA-matched embryo is found.
FAQs
Q. Is HLA matching allowed everywhere?
Ans : Availability varies by region, clinic policies, and ethical guidelines. Some countries restrict its use.
Q. Does PGT-A help with HLA matching?
Ans : No—PGT-A screens for aneuploidy. HLA compatibility is separate.
Q. Can we use donor sperm or donor eggs?
Ans : Yes, but it will reduce biological similarity and may lower match likelihood.
Q. What if we don’t get an HLA-matched embryo?
Ans : Options include repeating IVF, using alternative donors, or proceeding with transplant strategies that don’t require full match.
Q. Is this considered “designer baby” technology?
Ans : No—clinics limit HLA matching to medically necessary transplant scenarios, and oversight bodies regulate ethical boundaries.
Next Steps
- Free 15-min nurse consult
- Upload your labs
- Get a personalized cost breakdown for your case
Related Links

Dr. Kulsoom Baloch
Dr. Kulsoom Baloch is a dedicated donor coordinator at Egg Donors, leveraging her extensive background in medicine and public health. She holds an MBBS from Ziauddin University, Pakistan, and an MPH from Hofstra University, New York. With three years of clinical experience at prominent hospitals in Karachi, Pakistan, Dr. Baloch has honed her skills in patient care and medical research.