Glossary — Common Financial and Insurance Terms in a simplified reference for decoding the language behind coverage, billing, financing, and clinic estimates. It explains where each term fits in your journey, how it shapes cost and timing, and why being precise with language prevents major downstream problems.
Who It Helps
This resource is a strong fit if you:
- Are navigating insurance for the first time in fertility care
- Receive estimates or bills you don’t fully understand
- Want to compare clinics, financing options, or employer benefits
- Need confidence when discussing costs with financial coordinators
- Hate being surprised by billing differences between “allowed,” “charged,” and “covered”
Less needed if you already have comprehensive fertility coverage with minimal out-of-pocket responsibility or a bundled package with fixed pricing.
Step-by-Step
How to use this glossary effectively:
- Skim all definitions once to catch the terms you’ve been hearing but didn’t fully understand.
- Flag terms tied to timing (deductible reset, prior authorization, out-of-pocket max).
- Flag terms tied to cash flow (coinsurance, copay, EOB, prepayment).
- Match glossary terms to your clinic estimate to catch gaps or assumptions.
- Use the glossary during insurance calls so you ask the right questions.
This small upfront clarity prevents month-long billing issues later.
Pros & Cons
Pros
- Replaces confusion with clarity
- Saves money by preventing billing errors
- Strengthens conversations with clinics and insurance
- Helps compare financing or packages accurately
Cons
- Does not change your actual coverage
- Some terms vary slightly across plans
- Can’t remove all uncertainty—insurance billing always has moving parts
Costs & Logistics
Understanding terms affects:
- When you pay
- How much you pay
- What is reimbursable
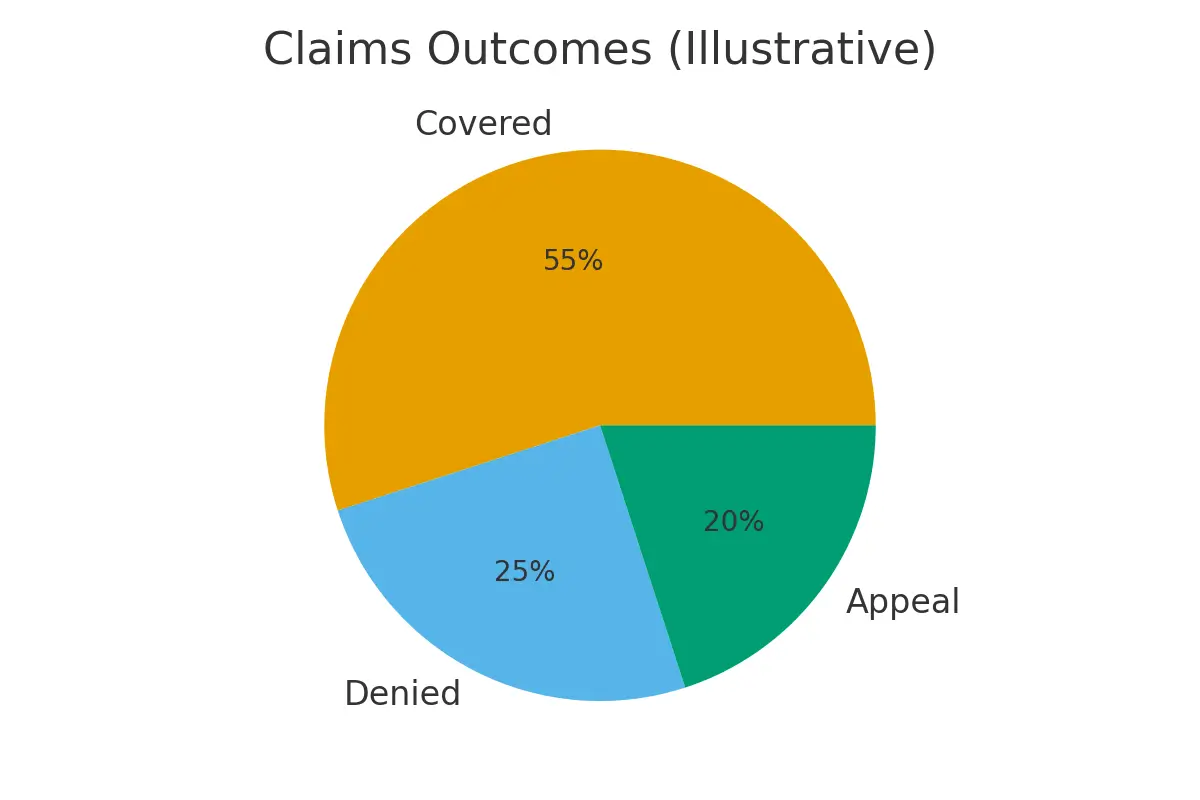
- Whether a claim is approved or denied
- How clinic estimates differ from insurance calculations
Key intersections:
- Prior authorization determines whether a cycle can start
- Deductible and OOP max determine when you shift from paying thousands to paying little or nothing
- Allowed amount determines your true responsibility
- Coordination of benefits matters when you have employer coverage plus secondary insurance
Good comprehension reduces stress during high-stakes phases like stimulation starts, retrieval, transfer, or surrogacy milestones.
What Improves Outcomes
What actually makes a difference:
- Asking for itemized estimates before committing
- Confirming prior authorization in writing
- Reviewing EOBs regularly to catch errors early
- Planning cycles around deductible resets
- Understanding which codes your clinic uses for billing
What rarely matters:
- Memorizing every insurance clause
- Focusing on small dollar differences rather than the big drivers (meds, cycle fees, lab work)
- Over-optimizing when coverage already caps your costs
Case Study — Clearing Confusion with Five Terms
A patient starting IVF kept receiving different price estimates—from $6,500 to $13,000—and couldn’t understand why.
Once they reviewed five terms:
- Deductible (not yet met)
- Allowed amount (much lower than clinic cash pay price)
- Coinsurance (20% until reaching OOP max)
- Prior authorization (required for the lab portion)
- OOP max (only $3,500 away)
The picture suddenly made sense:
They’d pay high out-of-pocket for the first procedure, then almost nothing thereafter.
They timed their retrieval early in the year, hit their out-of-pocket max, and their next transfer cost $0.
The path from confusion to clarity came from understanding definitions—not changing their medical plan.
Mistakes to Avoid
- Assuming “covered” means “free”
- Not checking whether prior authorization is needed
- Confusing charged vs allowed amounts
- Ignoring EOBs and letting errors snowball
- Starting a cycle right before deductible reset
- Believing verbal insurance answers without written confirmation
- Not asking the clinic which CPT codes they will use
FAQs
Q. Is an insurance “estimate” the same as what I’ll actually pay?
Ans : No. It’s a projection. Actual cost depends on claims, coding, and allowed amounts.
Q. What’s the difference between a copay and coinsurance?
Ans : A copay is a fixed amount; coinsurance is a percentage of the allowed amount.
Q. Why does my clinic say one price and my insurance says another?
Ans : Clinics quote retail rates. Insurance calculates based on contracted (allowed) rates.
Q. What does an EOB do for me?
Ans : It confirms what was billed, what insurance paid, and what you truly owe.
Q. When do prior authorizations matter most?
Ans : Before IVF, lab procedures, genetic testing, donor services, and surrogacy milestones. Starting without it risks denial.
Next Steps
- Free 15-min nurse
- consult Upload your labs for review
- Get a personalized cost breakdown for your case
Related Links
- Financing insurance benefits
- Intended Parents
- Become a Surrogate
- Fixed‑Cost Packages
- SART
- CDC ART
- ASRM

Dr. Kulsoom Baloch
Dr. Kulsoom Baloch is a dedicated donor coordinator at Egg Donors, leveraging her extensive background in medicine and public health. She holds an MBBS from Ziauddin University, Pakistan, and an MPH from Hofstra University, New York. With three years of clinical experience at prominent hospitals in Karachi, Pakistan, Dr. Baloch has honed her skills in patient care and medical research.