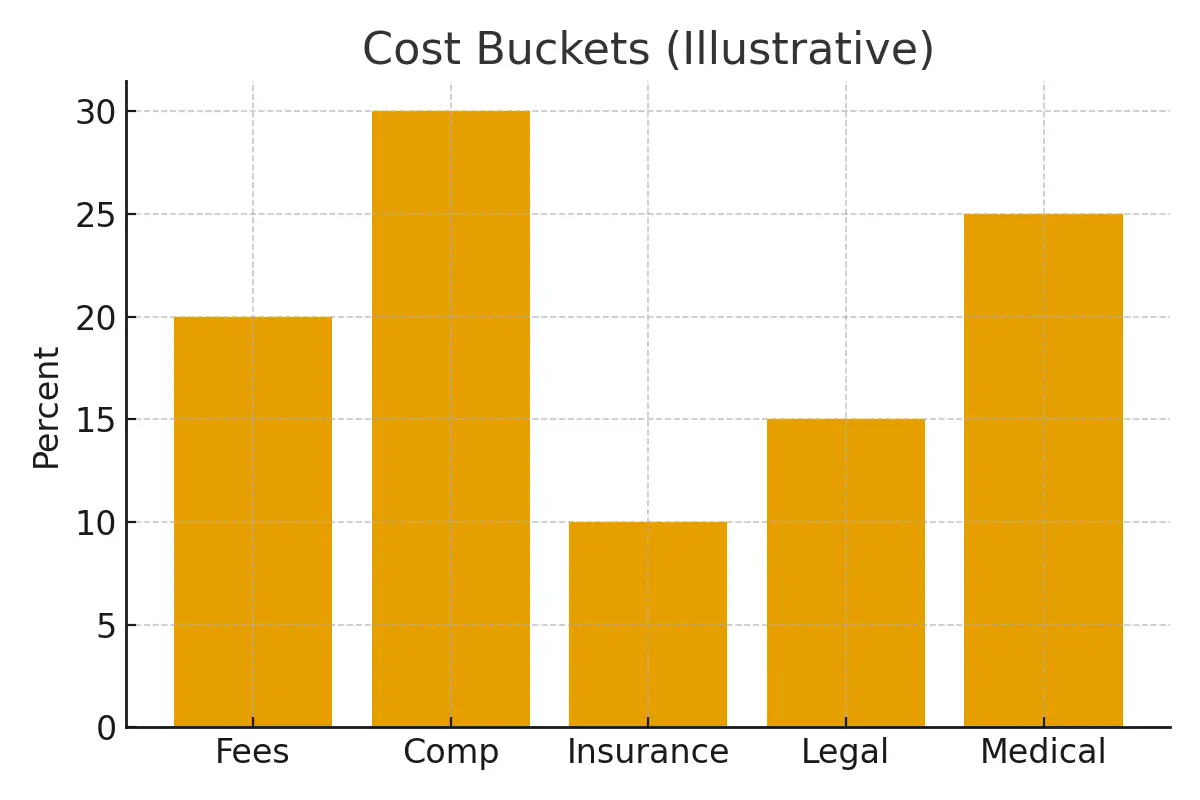
A side-by-side look at how different budgets change what’s possible in fertility care and family-building. It shows how upstream choices—clinic selection, insurance use, medication sourcing, financing, donor/surrogacy planning—directly affect downstream results, cash-flow, and emotional stress.
You’ll see how families adapt within budgets ranging from lean, moderate, to expansive, and what trade-offs consistently matter most.
Who It Helps
This guide is a good fit if you:
- Aren’t sure whether your budget is “enough” for your chosen path
- Want realistic expectations before committing to loans, donor programs, or surrogacy
- Need to compare insurance vs self-pay routes
- Want to avoid repeating hidden mistakes others learned the hard way
It may be less helpful if you already have full employer coverage, unlimited cycles, or a pre-negotiated surrogacy/egg-donor package with fixed payments.
Step-by-Step
A simple sequence for evaluating your situation:
- Define your 12–18 month budget band (lean / moderate / expansive).
- Map what’s included—coverage limits, meds, out-of-network rules, deductibles, donor/surrogacy components.
- Match this to a pathway—IUI, IVF, donor eggs, donor sperm, embryo banking, surrogacy.
- Add timing checkpoints—insurance resets, open enrollment, escrow milestones, legal steps.
- Pressure-test the plan for best-case, mid-case, and worst-case outcomes.
- Decide early how you’ll adapt if results differ (e.g., when to switch from own eggs to donor).
Pros & Cons
Pros
- Brings clarity through real examples
- Helps set boundaries on spending before emotional decisions hit
- Improves confidence in financial planning
- Highlights patterns that consistently reduce risk
Cons
- Real-world examples can’t perfectly match every situation
- Case studies simplify complexities (labs, medical nuance, legal variability)
- Costs vary widely by region, clinic, and individual biology
Costs & Logistics
Across budgets, the most variable line items include:
- Clinic consults and cycle fees
- Medications (huge range depending on ovarian response)
- Donor sperm or donor egg costs
- Genetic testing and storage fees
- Surrogacy: legal, insurance, escrow, compensation, medical care
- Monitoring: in-network vs out-of-network differentials
- Timing: calendar year resets can add $3k–$12k unexpectedly
Case studies later show how these stack up differently based on available funds.
What Improves Outcomes
Actions that meaningfully change results across all budgets:
- Choosing a clinic with strong experience for your age/diagnosis
- Aligning financial planning with biology (e.g., faster action at older ages)
- Early genetic counseling to avoid later, costly detours
- Running all insurance pre-authorizations before starting
- Asking for itemized billing to prevent expensive errors
- Keeping a timeline calendar tied to coverage resets and deductible rules
What rarely changes outcomes:
- Switching programs based on small price differences
- Delaying to “save more” when age-related decline is steep
- Paying extra for add-ons not supported by evidence
Case Study — Three Budgets, Three Paths
1. Lean Budget: $8,000–$15,000 Total
Challenge: Diminished reserve, no IVF coverage.
Choices:
- One self-pay IVF cycle was too risky financially.
- Chose two IUIs + medication coupons, strict calendar planning.
- Bought one donor sperm vial upfront to lock price.
Outcome: Pregnant on second IUI; total spend $9,800.
Key insight: Simplicity and discipline prevented overspending on low-probability options.
2. Moderate Budget: $25,000–$45,000 Total
Challenge: Age 37, failed IUIs, partial insurance.
Choices:
- Maximized insurance for diagnostics + monitoring
- One stim IVF cycle, froze 3 embryos
- Deferred PGT-A until after retrieval to spread costs
- Used 0%-APR financing for medications only
Outcome: Transferred embryo #2 and delivered.
Key insight: Strategic sequencing (insurance first, retrieval next) stretched the budget.
3. Expansive Budget: $120,000–$180,000 Total
Challenge: Needed both donor eggs and gestational carrier.
Choices:
- Selected proven donor
- Locked a surrogacy agency’s fixed-fee package
- Added extra escrow buffer
- Purchased insurance rider for surrogate maternity care
Outcome: Smooth timeline with minimal unexpected costs.
Key insight: Paying more for predictability reduced stress, legal risk, and delays.
Mistakes to Avoid
- Treating each bill as separate instead of creating a single 18-month plan
- Ignoring insurance timing (deductibles, out-of-pocket max, open enrollment)
- Assuming cheaper cycles are better cycles
- Not adjusting when biology sends new signals
- Under-budgeting for medications
- Forgetting legal and escrow timelines for donor/surrogacy arrangements
FAQs
Q. How do I know if my budget is “enough”?
Ans : Map it to the expected cost of the path you’re considering. Case studies help show the realistic bands for IUI, IVF, donor eggs, and surrogacy.
Q. Should I choose a cheaper clinic if money is tight?
Ans : Only if the success rates for your age/diagnosis are comparable. Saving $3,000 but lowering odds is a false economy.
Q. Can I mix insurance and self-pay?
Ans : Yes—many families do. Often diagnostics are insurance-friendly but procedures are cheaper as cash pay.
Q. How much buffer should I add?
Ans : Most families underestimate by 15–25%. A buffer covers meds, cycle changes, extra visits, or legal/admin steps.
Q. When do people decide to switch from own-egg IVF to donor eggs?
Ans : Usually after one failed or poor-yield cycle if their age or reserve suggests rapidly declining odds. Budget, urgency, and medical advice drive the switch.
Next Steps
- Free 15-min nurse
- consult Upload your labs for review
- Get a personalized cost breakdown for your case
Related Links
- Financing insurance benefits
- Intended Parents
- Become a Surrogate
- Fixed‑Cost Packages
- SART
- CDC ART
- ASRM

Dr. Kulsoom Baloch
Dr. Kulsoom Baloch is a dedicated donor coordinator at Egg Donors, leveraging her extensive background in medicine and public health. She holds an MBBS from Ziauddin University, Pakistan, and an MPH from Hofstra University, New York. With three years of clinical experience at prominent hospitals in Karachi, Pakistan, Dr. Baloch has honed her skills in patient care and medical research.