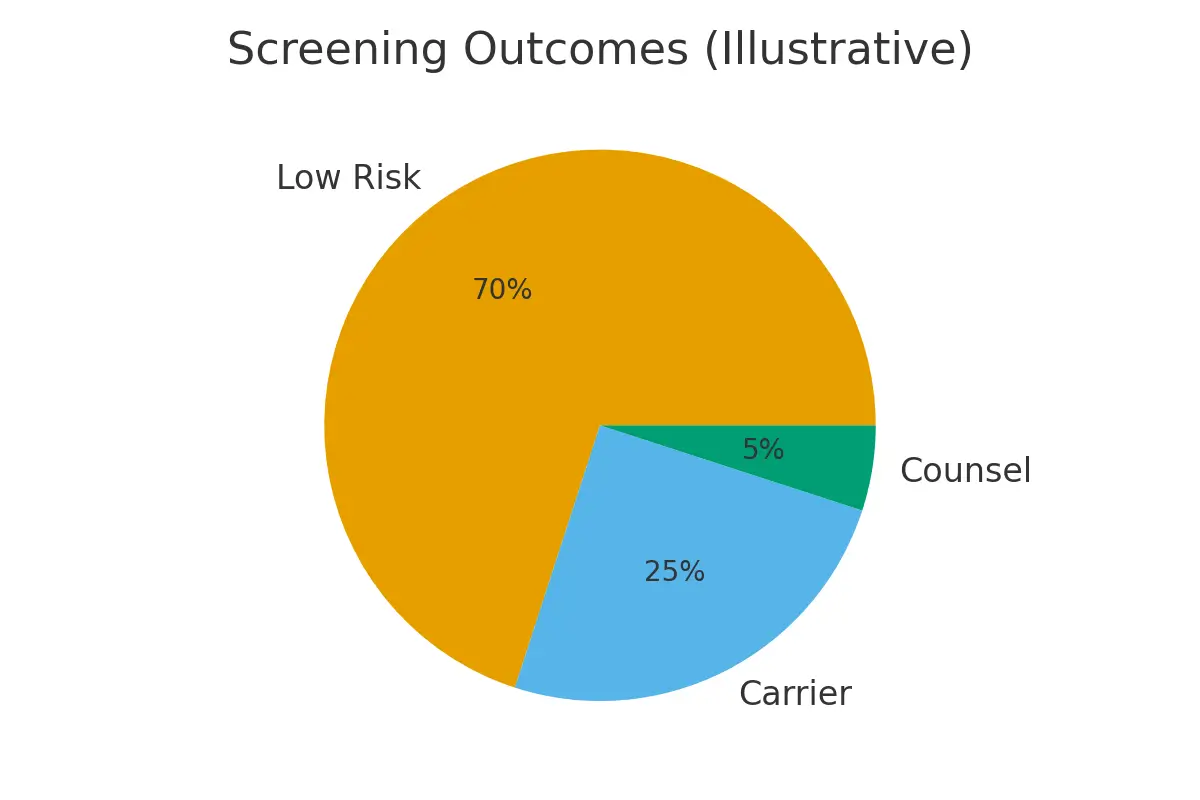
Expanded carrier screening tests your DNA for hundreds of inherited conditions — usually recessive or X-linked disorders — that you could pass on to a future child.
ECS helps answer three simple questions:
- Are you a carrier of any inherited condition?
- If you are, is your partner also a carrier of the same condition?
- If both partners carry the same condition, what’s the actual risk to a pregnancy and what are the options?
What ECS does not do:
- Diagnose disease in you — carriers are typically healthy
- Guarantee an unaffected child
- Replace diagnostic prenatal testing
- Predict every genetic condition (no test covers everything)
Where it fits:
- Early in preconception or IVF planning
- Before embryo creation if PGT-M might be needed
- Before pregnancy to avoid surprises during prenatal screening
Upstream decisions — like panel size, your ancestry, how the partner is tested, or whether results are reviewed before IVF — directly influence downstream options and timing.
Who It Helps
Signals of Good Fit vs When to Choose Another Path
Good Fit Signals
ECS is particularly helpful when:
- You’re planning IVF and want to know which genetic panels matter before creating embryos
- You’re unsure of family medical history
- One partner is from a population with higher carrier rates
- There is a history of miscarriages or infant loss that might have a genetic cause
- You want to identify if PGT-M could prevent passing on a serious condition
- You want to avoid last-minute decisions during pregnancy
Less Helpful or Gray Zones
ECS may provide limited usefulness if:
- A known familial mutation already exists (a targeted single-gene test may be enough)
- You or your partner decline DNA testing
- You have very limited time before a planned transfer (results can take 2–4 weeks)
- You expect no change in your plan regardless of results
- Your ancestry makes certain rare conditions extremely unlikely and targeted panels may suffice
Age, ovarian reserve (AMH/AFC), semen parameters, and clinical history shape whether ECS should be paired with PGT-M or simply used for preconception awareness.
Step-by-Step
A Simple Sequence With Timing Checkpoints
-
Genetic Counseling or Ordering Panel
– Choose panel size; confirm the lab and insurance requirements. -
Sample Collection (Blood or Saliva)
– Testing typically takes 2–4 weeks. -
Partner Testing
– Performed only if the first partner is a carrier, or both partners test at the same time. -
Results Review
– Outcomes:
• No shared conditions → standard preconception or IVF pathway
• Shared recessive condition → consider PGT-M
• X-linked carrier → discuss specific risks and IVF options -
Integrate Findings Into Reproductive Plan
– IVF? PGT-M? Prenatal screening? Timing changes?
Setting these checkpoints prevents rushed decisions and helps coordinate IVF cycles without delays.
Pros & Cons
Balanced View of Benefits and Trade-offs
Pros
- Identifies risks before pregnancy
- Enables planning for PGT-M if both partners carry the same condition
- Reduces the chance of unexpected prenatal findings
- Particularly useful for couples with incomplete family history
- Often covered by insurance for one or both partners
Cons / Limitations
- Results can feel overwhelming if many carrier findings are listed
- Some findings have uncertain significance
- Can add 2–4 weeks to the timeline if not planned early
- Not every condition is testable or perfectly detectable
- Raises anxiety even when risks are low
Costs & Logistics
Avoiding Surprise Bills
Typical cost considerations:
- Panel testing fee (varies by lab and insurance)
- Partner testing (may be discounted or free if needed)
- Genetic counselor consult
- Add-on testing for variants of uncertain significance
- Potential follow-up testing for relatives
To stay organized:
- Confirm whether your plan requires prior authorization
- Track what is billed to insurance vs self-pay
- Ask which partner should test first to avoid unnecessary cost
- Use a simple tracker to record result dates and follow-ups
- Clarify turnaround times to avoid delaying IVF or transfer dates
What Improves Outcomes
Actions That Materially Change Results (and Those That Rarely Do)
High-Impact Actions
- Testing both partners when one carries a recessive mutation
- Ordering the panel before starting IVF
- Reviewing results with a genetic counselor
- Securing all DNA samples needed for PGT-M before stimulation
- Coordinating timelines so ECS results don’t delay retrieval or transfer
Low-Impact or Low-Yield Actions
- Repeating ECS panels without new clinical information
- Testing embryos when no shared condition requires PGT-M
- Overreacting to single-carrier findings without partner testing
- Assuming ECS detects everything — it doesn’t cover all rare disorders
Case Study
From Uncertainty to Clarity Using Steady Communication and Defined Thresholds
A couple preparing for IVF completed expanded carrier screening. The woman’s panel showed she was a carrier of a recessive metabolic disorder; her partner’s panel confirmed he was too. They felt overwhelmed by the implications.
Through:
- A genetics consult clarifying inheritance risks
- Early planning so the IVF cycle wasn’t delayed
- Creating a threshold: “Proceed with PGT-M only if ≥3 blastocysts are available”
- Cost tracking and upfront discussions on lab fees
- Weekly timeline check-ins
They moved from panic to a clear plan. Their IVF cycle produced four blastocysts, PGT-M identified two unaffected embryos, and the transfer plan became straightforward and calm.
Mistakes to Avoid
Common Traps + Simple Fixes
- Testing too late (delays IVF timelines)
- Not testing the partner when one is a carrier
- Confusing carrier status with having the disease
- Assuming a long list of findings = high risk (usually, it doesn’t)
- Overlooking the need for PGT-M probe development time
- Not planning for insurance coverage or out-of-pocket costs
- Expecting ECS to replace prenatal screening
FAQs
Q. If I’m a carrier, does that mean I have the disease?
Ans : No — carriers are healthy and rarely show symptoms.
Q. What if we both carry the same recessive condition?
Ans : You have a 25% chance per pregnancy of having an affected child; IVF with PGT-M can help reduce that risk.
Q. How long do results take?
Ans : Usually 2–4 weeks depending on the lab.
Q. Should everyone do expanded carrier screening?
Ans : Increasingly yes, but smaller panels may be enough in certain cases.
Q. Do we need PGT-A as well?
Ans : Depends on age, embryo numbers, and clinical history. They serve different purposes.
Next Step
- Free 15-min nurse consult
- Upload your labs for a personalized review
- Receive a customized cost breakdown for your case
Related Links

Dr. Kulsoom Baloch
Dr. Kulsoom Baloch is a dedicated donor coordinator at Egg Donors, leveraging her extensive background in medicine and public health. She holds an MBBS from Ziauddin University, Pakistan, and an MPH from Hofstra University, New York. With three years of clinical experience at prominent hospitals in Karachi, Pakistan, Dr. Baloch has honed her skills in patient care and medical research.